What Is PCOS?
Polycystic ovary syndrome (PCOS) is a common condition that affects women and influences how our ovaries work. Around one in ten women in the UK suffer from PCOS.
Clinicians use the Rotterdam criteria to diagnose PCOS. (1) In order to be diagnosed you need to be suffering from two of the following:
- Oligo- or anovulation – irregular or lack of ovulation.
- Clinical and/or biochemical signs of hyperandrogenism– excessive hormones such as testosterone that may cause excessive body or facial hair, acne, hair loss and inflamed skin.
- Polycystic ovaries – fluid filled sacs on the ovaries.
The term polycystic ovary syndrome is actually a little misleading, as you only need to be experiencing two of the three to be diagnosed with PCOS. This means you can still have PCOS without having polycystic ovaries. If you have any concerns and think you may have PCOS it is best to consult your doctor. In some cases PCOS can affect fertility because it impacts hormone levels and ovulation.
What Are The symptoms?
Symptoms of PCOS usually become clear in a woman’s late teens and early 20s. These include: irregular/no periods, struggling to conceive, excessive hair growth, weight gain, thinning hair and oily skin/acne.
What Causes PCOS?
It is unclear exactly what causes PCOS, but there is thought to be a genetic link as it can run in families. (2) The condition is characterised by abnormally high hormone levels in the body, such as the hormone insulin. Insulin plays a role in controlling our blood sugar. Those who suffer from PCOS are often insulin resistant and therefore produce high levels of insulin to combat its ineffectiveness – carrying extra weight, particularly around the middle, can further exacerbate this. A higher level of insulin contributes to an increase in the production and activity of hormones such as testosterone.
Nutrition & PCOS

Weight Loss
The insulin resistance that is associated with PCOS, can make it harder to lose weight and can also result in the development of type II diabetes and other metabolic diseases.
Whilst there is no cure for PCOS, there are dietary changes that you can make to manage PCOS and these changes can help to reduce some of the symptoms associated with PCOS. If you are overweight, losing weight may help you to reduce and manage your symptoms . In fact, a weight loss of 5-10% can significantly improve symptoms. (3)
If you wish to lose weight, it is advisable that you do this in a sensible way. You can achieve this by gradually reducing your calorie intake. Small dietary swaps and reducing your portion sizes can help you to achieve this. In addition, you can become more physically active – which will help you to burn up more energy.
Low Glycaemic Index
Consuming low glycaemic index (GI) foods can help to improve insulin levels which is beneficial for controlling the symptoms of PCOS. (4)
When insulin is higher this can result in abnormal levels of testosterone. In women, elevated testosterone levels can result in the physical symptoms of PCOS, which include acne, excess hair growth and irregular periods. Consuming a low GI diet may help you to manage the symptoms of PCOS as well as help with weight loss.
What Is Low Glycaemic Index?
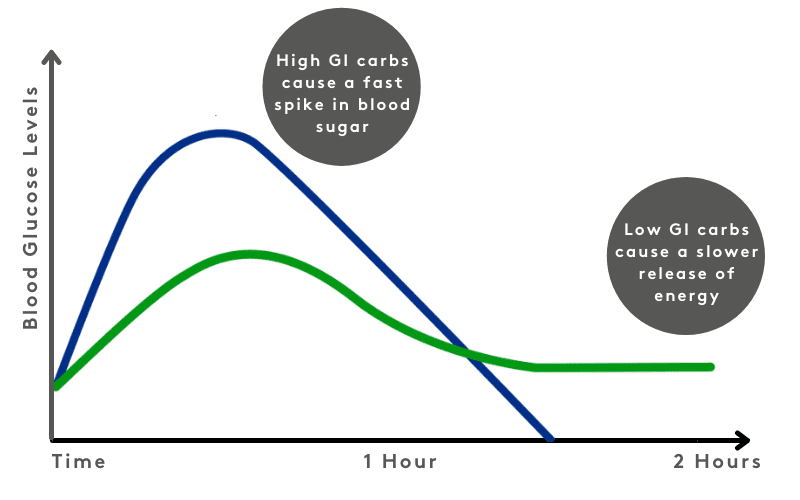
The GI is a ranking system, which shows how quickly your blood glucose (sugar) increases after eating different carbohydrates.
Low GI diets raise blood glucose levels more slowly. The Mediterranean diet can help you to consume a lower GI dietary pattern; as it focuses on consuming whole grain and less processed carbohydrates as opposed to refined carbohydrates, the former generally being of a lower GI.
Fruit and vegetables generally have a low glycaemic index, so remember to aim for at least 5 portions of fruit and vegetables per day. Opt for more vegetables than fruit as vegetables have a lower sugar content so trigger less of an insulin response.
Lower Carbohydrate Intake
A lower carbohydrate intake and higher intake of unsaturated fats may also help to lower insulin levels and thus testosterone levels in women with PCOS. (5) Therefore you may wish to lower your carbohydrate intake by reducing portion sizes of carbohydrates such as; bread, cereal, pasta etc. However, very low carbohydrate diets may not be sustainable in the long term, and often lack fibre. So try to find a balance that works for you.
Fats
It is advisable to keep fat intake to less than <30% of total calories a day, with a low proportion of saturated fats. (6) Reducing your saturated fat intake can also help to reduce inflammation. Unsaturated fats such as omega-3 fatty acids which are found in fish, may help to improve insulin resistance and inflammation in women with PCOS. (7)
Protein
A moderate increase in protein intake may help you to feel fuller for longer; as well as manage your blood sugar. (8) You can ensure that you are consuming enough protein by consuming; lean meat and fish as well as plant-based alternatives such as tofu, soy-based alternatives, beans, lentils, quinoa and nuts.
Summary
PCOS is one of the most common reproductive and metabolic disorders in women. There are plenty of dietary changes that you can make to help to manage your PCOS, however if you do have any concerns it is best to speak to your GP or a Registered Dietitian.
- Losing weight may help if you are overweight – even 5-10% weight loss can offer significant improvements to your symptoms.
- Replacing saturated fats with unsaturated fats – can help you to improve insulin resistance and reduce inflammation.
- Carbohydrates – Choosing low glycaemic index carbohydrates can help to manage insulin levels, which can help you to manage testosterone levels, and you should avoid a high carbohydrate intake.
- Protein – Protein can help to manage hunger and blood sugar levels.
- Fauser BCJM. Revised 2003 consensus on diagnostic criteria and long-term health risks related to polycystic ovary syndrome. Fertil Steril [Internet]. 2004;81(1):19–25. Available from: https://pubmed.ncbi.nlm.nih.gov/14711538/
- Morgante G, Cappelli V, Di Sabatino A, Massaro MG, De Leo V. Polycystic ovary syndrome (PCOS) and hyperandrogenism: the role of a new natural association. Minerva Ginecol. 2015 Oct;67(5):457-63. PMID: 26491824.
- Fong S, Douma A, Verhaeghe J. Implementing the international evidence-based guideline of assessment and management of polycystic ovary syndrome (PCOS): how to achieve weight loss in overweight and obese women with PCOS? J Gynecol Obstet Hum Reprod. 2021 Jun;50(6):101894. doi: 10.1016/j.jogoh.2020.101894. Epub 2020 Aug 16. PMID: 32814159.
- Marsh KA, Steinbeck KS, Atkinson FS, Petocz P, Brand-Miller JC. Effect of a low glycemic index compared with a conventional healthy diet on polycystic
- Perelman D, Coghlan N, Lamendola C, Carter S, Abbasi F, McLaughlin T. Substituting poly- and mono-unsaturated fat for dietary carbohydrate reduces hyperinsulinemia in women with polycystic ovary syndrome. Gynecol Endocrinol. 2017 Apr;33(4):324-327. doi: 10.1080/09513590.2016.1259407. Epub 2016 Dec 2. PMID: 27910718.
- Farshchi, A. Rane, A. Love & R. L. Kennedy (2007) Diet and nutrition in polycystic ovary syndrome (PCOS): Pointers for nutritional management, Journal of Obstetrics and Gynaecology, 27:8, 762-773, DOI: 1080/01443610701667338
- Li J, Armstrong CL, Campbell WW. Effects of Dietary Protein Source and Quantity during Weight Loss on Appetite, Energy Expenditure, and Cardio-Metabolic Responses. Nutrients. 2016 Jan 26;8(2):63. doi: 10.3390/nu8020063. PMID: 26821042; PMCID: PMC4772027.
- Oner G, Muderris II. Efficacy of omega-3 in the treatment of polycystic ovary syndrome. J Obstet Gynaecol. 2013 Apr;33(3):289-91. doi: 10.3109/01443615.2012.751365. PMID: 23550861.

